National Center for research on survivorship and Late Adverse Effects after Cancer in the Pelvic Organs.
The Research Center has been granted by the Danish Cancer Society.
Closely linked to the research center is clinical centers granted by Region Nordjylland and Region Midtjylland. It involves all parts of Denmark, but is centered at Aarhus University Hospital and Aalborg University Hospital.
To perform prospective observational and randomized studies to improve the knowledge regarding risk and treatment of sequelae to colorectal/anal/bladder/cervical/prostate cancer.
The studies will be performed in close collaboration with the relevant national Danish multidisciplinary cancer group.
- Peter Christensen, Professor, dr.med. Aarhus University Hospital (Chairman of the research center and the surgical clinical center in Aarhus)
- Søren Laurberg, Professor, dr.med. Aarhus University
- Klaus Krogh, Professor, dr.med. Aarhus University Hospital
- Asbjørn M. Drewes, Professor, dr.med. Aalborg University Hospital
- Katrine Emmertsen, Senior consultant, Ph.D.Randers Hospital
- Janne Fassov, Consultant, Ph.D. Aarhus University Hospital
- Therese Juul, Associate Professor, Ph.D. Nurse, Aarhus University Hospital

Haas, S., Faaborg, P. Liao, D., Laurberg, S., Gregersen, H., Lundby, L., Christensen, P. and Krogh, K. (2018). Anal sphincter dysfunction in patients treated with primary radiotherapy for anal cancer: a study with the functional lumen imaging probe. Acta Oncologica. 57,(4):465 - 472.
Juul, T., Elfeki, H., Christensen, P., Laurberg S., Emmertsen K.J., Bager, P. (2018). Normative Data for the Low Anterior Resection Syndrome Score (LARS Score). Annals of Surgery
Damsgaard, B., Dalby, H. R., Krogh, K., Jørgensen, S. M. D., Arveschough, A. K., Agnholt, J., Dahlerup, J. F. and Jørgensen, S. P.(2018). Long-term effect of medical treatment of diarrhoea in 377 patients with SeHCAT scan diagnosed bile acid malabsorption from 2003 to 2016; a retrospective study . Alimentary Pharmacology & Therapeutics. 47(7):951-957
Haas, S., Faaborg, P., Gram, M., Lundby, L., Brock, C., Drewes, A. M., Laurberg, S., Krogh, K. and Christensen, P.(2018). Abnormal neuronal response to rectal and anal stimuli in patients treated with primary radiotherapy for anal cancer. Radiotherapy and Oncology, 128:369–374.
Jørgensen, J.B., Bondeven, P., Iversen L.H., Laurberg S. og Pedersen, B.G. (2018). Pelvic insufficiency fractures frequently occur following preoperative chemo-radiotherapy for rectal cancer – a nationwide MRI study. Colorectal Dis. 20 (10):873-880
Yde, J., Larsen, H. M., Laurberg, S., Krogh, K. and Møller, H. B.(2018). Chronic diarrhoea following surgery for colon cancer—frequency, causes and treatment options. Int. J. Colorectal Dis. 33 (6):683–694
Thyø, A., Emmertsen, K.J. and Laurberg S.(2018). The Rectal Cancer Female Sexuality Score: Development and Validation of a Scoring System for Female Sexual Function After Rectal Cancer Surgery. Diseases of the Colon & Rectum. 61(6):656–666
Bertelsen, C.A. , Effeki, H., Neuenschwander, A.U., Laurberg S., Kristensen, B., and Emmertsen, K.J.(2018). The risk of long-term bowel dysfunction after resection for sigmoid adenocarcinoma: a cross sectional survey comparing complete mesocolic excision with conventional surgery. Colorectal Dis. 20:256-266
Jakobsen, I.H., Jeppesen, M.M., Simard, S., Thaysen, H.V., Laurberg, S. and Juul, T.(2018). Initial validation of the Danish version of the Fear of Cancer Recurrence Inventory (FCRI) in colorectal cancer patients. J. of Cancer Survivorship. 12(6):723-732
Elfeki H, Thyø A, Nepogodiev D, Pinkney TD, White M, Laurberg S, Christensen P and the Colostomy Impact Study Group.(2018). Patient and healthcare professional perceptions of colostomy-related problems and their impact on quality of life following rectal cancer surgery. BJS Open.2(5):336-344
Mortensen, A.R., Thyø, A., Emmertsen, K.J. and Laurberg. S.(2018). Chronic pain after rectal cancer surgery-development and validation of a scoring system. Colorectal Dis. 21:90-99
Elfeki, H., Larsen, H.M., Emmertsen, K.J., Christensen, P., Youssef, M., Khafagy, W.,Omar, W.and Laurberg. S.(2019). Bowel dysfunction after sigmoid resection for cancer and its impact on quality of life. BJS. 106:142-151
Kristensen H Ø, Thyø A, Christenensen P. (2019). Systematic review of the impact of demographic and socioconomic factors on quality of life i ostemized colorectal cancer survivors. Acta. Onco. 58(5): 566-572
Kronborg C, Serup-Hansen E, Wind K, Christensen P, Spindler K (2019). Patient - reported outcomes including LARS score and quality of life one year after chemoradiotherapy for anal cancer. Ann Oncol. 30. Suppl 4:iv61.
M-L Feddern, K J Emmertsen, S Laurberg (2019). Quality of life with or without sphincter preservation for rectal cancer. Colorectal Dis. 21(9):1051-1057
A Thyø, H Elfeki, S Laurberg, K J Emmertsen (2019). Female sexual problems after treatment for colorectal cancer - a population-based study. Colorectal Dis 21(10):1130-1139.
C Keane, N S Fearnhead, L Bordeianou, P Christensen, E Espin Basany, S Laurberg, A Mellgren, C Messick, G R Orangio, A Verjee, K Wing, I Bissett, LARS International Collaborative Group (2020). International consensus definition of low anterior resection syndrome. Colorectal Dis 22(3):331-341
K K Jensen, K J Emmertsen, S Laurberg, P-M Krarup (2020). Long-term impact of incisional hernia on quality of life after colonic cancer resection. Hernia 24(2):265-272.
A Thyø, S Laurberg, K J Emmertsen (2020). Impact of bowel and stoma dysfunction on female sexuality after treatment for rectal cancer. Colorectal Dis 22(8):894-905.
Helene Mathilde Larsen , Hossam Elfeki , Katrine Jøssing Emmertsen & Søren Laurberg (2020). Long-term bowel dysfunction after right-sided hemicolectomy for cancer. Acta Oncologica 2020, Vol. 59, No. 10, 1240–1245
Søren Laurberg, Therese Juul, Peter Christensen, Katrine Jøssing Emmertsen (2021). Time for a paradigm shift in the follow-up of colorectal cancer. Colorectal Dis 2021;23:341–344.
Jens Reumert Laurberg MD, Ph.D. and Viktoria Reumert Laurberg RN, MSc, Hossam Elfeki, MD, MSc, Jørgen Bjerggaard Jensen MD, DMSc, and Katrine J. Emmertsen MD, Ph.D. (2021). Male erectile function after treatment for colorectal cancer – a population-based cross-sectional study. Colorectal Dis 2021;23:367–375.
P Dalsgaard, K J Emmertsen, M Mekhael, S Laurberg, P Christensen (2021). Nurse-led standardized intervention for low anterior resection syndrome. A population-based pilot study. Colorectal Dis 2021;23:434–443.
Paul F Vollebregt, Lukasz Wiklendt, Daphne Ang, Mary L Venn, Mira Mekhael, Peter Christensen, Phil G Dinning, Charles H Knowles, S Mark Scott (2021).Altered anal slow-wave pressure activity in low anterior resection syndrome: short case series in two independent specialist centres provide new mechanistic insights. Colorectal Dis 2021;23:444–450.
Felipe F Quezada-Diaz, Hossam Elfeki, Katrine J Emmertsen, Emmanouil P Pappou, Rosa Jimenez-Rodriguez, Sujata Patil, Søren Laurberg (2021). Comparative analysis of the Memorial Sloan Kettering Bowel Function Instrument and the Low Anterior Resection Syndrome Questionnaire for assessment of bowel dysfunction in rectal cancer patients after low anterior resection. Colorectal Dis 2021;23:451–460.
Peter Christensen, Coen Im Baeten, Eloy Espín-Basany, Jacopo Martellucci, Karen P Nugent, Frank Zerbib, Gianluca Pellino, Harald Rosen (2021). Management guidelines for Low Anterior Resection Syndrome the MANUEL project. Colorectal Dis 2021;23:461–475.
Saija Sinimäk,Hossam Elfeki, Marianne Højsgaard Kristensen, Søren Laurberg, Katrine J Emmertsen (2021). Urinary dysfunction after colorectal cancer treatment and impact on quality of life a national cross-sectional study in females. Colorectal Dis 2021;23:384–393.
Camilla J S Kronborg, Peter Christensen, Bodil G Pedersen, Karen-Lise G Spindler (2021). Anorectal function and radiation dose to pelvic floor muscles after primary treatment for anal cancer. Radiotherapy & Oncology
Marianne Højsgaard Kristensen, Hossam Elfeki, Saija Sinimäki, Søren Laurberg and Katrine J. Emmertsen (2021). Urinary dysfunction after colorectal cancer treatment and impact on quality of life – a national cross-sectional study in males. Colorectal Dis 2021;23:394–404.
Mira Mekhael, Helle Ø Kristensen, Helene Mathilde Larsen, Therese Juul, Anton Emmanuel, Klaus Krogh and Peter Christensen (2021). Transanal Irrigation for Neurogenic Bowel Disease, Low Anterior Resection Syndrome, Faecal Incontinence and Chronic Constipation: A Systematic Review. J. Clin. Med. 10, 753.
Therese Juul, Annette Boesen Bräuner, Asbjørn Mohr Drewes, Katrine Jøssing Emmertsen, Klaus Krogh, Søren Laurberg, Michael Bødker Lauritzen9, Ole Thorlacius- Ussing, Peter Christensen (2021). Systematic screening for late sequelae after colorectal cancer— a feasibility study. Colorectal Dis 2021;23:345–355.
Helene M. Larsen, Mira Mekhael, Therese Juul, Mette Borre, Peter Christensen, Asbjørn Mohr Drewes, Ole Thorlacius- Ussing, Søren Laurberg, Klaus Krogh, Janne Ladefoged Fassov (2021). Long- term gastrointestinal sequelae in colon cancer survivors: prospective pilot study on identification, the need for clinical evaluation and effects of treatment. Colorectal Dis 2021;23:356–366.
Pia Møller Faaborg, Susanne Haas, Donghua Liao, John Ploen, Anders Jakobsen, Hans Bjarke Rahr, Soeren Laurberg, Hans Gregersen, Lilli Lundby, Peter Christensen ,Klaus Krogh (2021). Long-term anorectal function in rectal cancer patients treated with chemoradiotherapy and endorectal brachytherapy. Colorectal Dis 2021:23(9):2311-2319
Mette Bach Larsen, Heidi Heinsen Bachmann, Bo Søborg, Tinne Laurberg, Katrine J. Emmertsen, Søren Laurberg, Berit Andersen (2021). Prevalence of self-reported abdominal symptoms among 50–74-years-old men and women eligible for colorectal cancer screening –a cross-sectional study. BMC cancer 2021; 21:910
Pernille Pedersen, Søren Laurberg, Niels Trolle Andersen, Ivan Steenstra, Claus Vinther Nielsen, Thomas Maribo, Therese Juul (2021).Prevalence of self-reported abdominal symptoms among 50–74-years-old men and women eligible for colorectal cancer screening –a cross-sectional study. BMC cancer2021; 21:910
Systematic screening

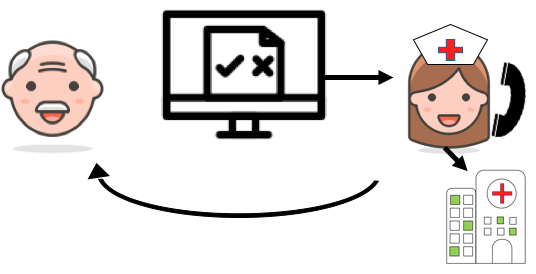
Since 2018 we have been performing a systematic screening of late sequelae that may develop after undergoing surgery for colorectal cancer (CRC). Via electronic surveys we aim at identifying all patients requiring treatment of late sequelae after CRC.
Surgically treated CRC patients receive a link to an online survey 3, 12, 24 and 36 months after surgery. Patients who have had a temporary diverting stoma also receive the survey, but 3 months after the stoma reversal. The survey can be completed on a computer, mobile phone or tablet. Patients who prefer a paper version will receive this. So far, we have obtained a very high response rate (80.5%) and 72.5% of the surveys have been completed electronically (https://pubmed.ncbi.nlm.nih.gov/33420746/). Furthermore, we are currently in the process of testing a mobile application (Journl) to see if this can be useful in data collection (https://www.journl.dk/).
Questionnaires

The survey consists of validated questionnaires and a number of ad hoc items covering all known, and potentially treatable, late sequelae after CRC. Both colon- and rectal patients answer questions about organ specific sequelae such as bowel function, quality of life, urinary- and sexual function, chronic pain and work. Furthermore, for patients that have undergone surgery for advanced CRC (cytoreductive surgery + hyperthermic intraperitoneal chemotherapy and pelvic exenteration) the survey in addition include questions regarding general and psychological sequelae such as fatigue, self-reported cognitive dysfunction, sleep troubles, anxiety, depression and 'fear of cancer recurrence'. Our results show that majority of patients present with 2 or more symptoms at a time.
Treatment of late sequelae
Patients who indicate organ specific late sequelae and an interest in being contacted, receive a call from the project nurse, who presents treatment options and refers to specialists, if relevant. For colon cancer surveys contact has so far been requested by approx. 19% of the patients and approx. 8.5% have been referred for treatment of late sequelae, primarily bowel dysfunction. For rectal cancer surveys contact has been requested by approx. 30% and 16% have been referred for treatment of late sequelae mainly bowel and sexual dysfunction. For the general/psychological late sequelae we are currently setting up a multidisciplinary team (MDT) late sequelae conference where patients can be referred to.
So far, we have treated late sequelae in patients who have undergone treatment for rectal cancer, colon cancer, gynecological cancer, prostate cancer and anal cancer.
Nationalt symposium om senfølger efter kræft - 6. maj 2022
Find mere information og tilmeld dig:
Hent invitationen:
Program for dagen: